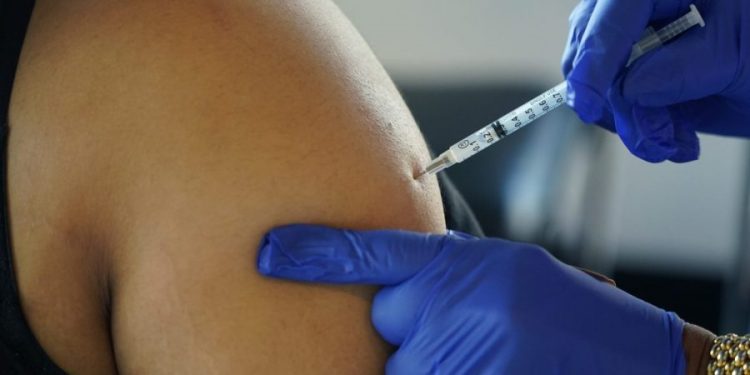
The Food and Drug Administration (FDA) approved updated COVID-19 shots on Monday for everyone 6 months and older in an effort to give Americans some added protection ahead of a potential winter uptick in infections.
Outside advisers for the Centers for Disease Control and Prevention (CDC) on Tuesday will recommend who should get the shots, which are manufactured by Moderna and Pfizer-BioNTech.
Once CDC Director Mandy Cohen signs off, the shots will be available to the public.
An application for an updated vaccine from Novavax, the only non-mRNA vaccine, is still pending. FDA referred questions to the company.
“Novavax is currently responding to the FDA’s requests to facilitate final review, and timing is ultimately at the discretion of the FDA,” the company said in a statement Monday, adding that doses of its vaccine have arrived in the U.S. for distribution should they receive regulatory clearances.
The updated COVID-19 shots will hit the market just as the U.S approaches the fall and winter respiratory virus season. They arrive along with new treatments to protect infants and older adults from respiratory syncytial virus (RSV).
“Vaccination remains critical to public health and continued protection against serious consequences of COVID-19, including hospitalization and death,” Peter Marks, director of the FDA’s Center for Biologics Evaluation and Research, said in a statement. “We very much encourage those who are eligible to consider getting vaccinated.”
The updated shots were designed to target the XBB.1.5 variant, which was dominant when vaccine makers began to formulate and test a new version. That variant is no longer dominant, though experts and administration officials have said the vaccines should still be effective at preventing severe infection against other variants that are circulating because they’re closely related.
It’s not yet clear which populations the shots will be considered for. Last year, the CDC’s advisory panel recommended only older and at-risk populations get the omicron-specific booster, but the agency decided instead to recommend everyone get the shots.
That recommendation “diluted the message” of who would most benefit from the shots, said Paul Offit, director of the Vaccine Education Center at Children’s Hospital of Philadelphia.
COVID-19 cases are rising, but the numbers are far below where they were at the height of the pandemic. Infections are not surging, and hospitals are far from being overwhelmed like they were at the height of the pandemic.
More than 95 percent of the U.S. population already has some level of COVID immunity, whether it’s from vaccination, infection or both. The new vaccine should provide the best protection for a few months before starting to wane, and will likely have the biggest impact on people who are older with underlying conditions, as well as some people who are immunocompromised.
The risks of serious illness for healthy younger people are low, though any infection carries a risk of turning into “long COVID,” when symptoms linger for months or even years later.
“It’s also important for people to realize that high level protection from the vaccine lasts on the order of three to four months, and it’s less clear what persists after that,” said Jesse Goodman, an infectious disease specialist and professor of medicine at Georgetown University.
“I think certainly, for the people at risk, it’s a clear cut advantage to get immunized, but for others, it’s a risk benefit decision,” Goodman said.
The Biden administration is refraining from calling the updated shots a booster, likely reflecting a concern that much of the public is vaccine-fatigued and has moved on from pandemic worries. Instead, it is being marketed as an annual shot, just like the flu vaccine.
“Barring the emergence of a markedly more virulent variant, the FDA anticipates that the composition of COVID-19 vaccines may need to be updated annually, as is done for the seasonal influenza vaccine,” the agency said Monday.
That messaging is also being echoed by the manufacturers.
“We appreciate the FDA’s timely review and encourage individuals who intend to get their flu shot to also get their updated COVID-19 vaccine at the same time,” said Stéphane Bancel, CEO of Moderna.
More than a year after the omicron boosters were rolled out, only about 17 percent of the public received a shot, and only about 43 percent of people over age 65.
The rollout of the newest shots is also complicated by the fact that they are no longer bought and distributed by the federal government, because the public health emergency expired in May.
That puts the burden of ordering shots on hospitals, physician offices and pharmacies, and on the public for paying for it.
Pfizer and Moderna have decided to charge up to $130 a shot, compared with $30 last year for the booster, which was produced under government contract.
People who have Medicare or private insurance likely won’t face any out of pocket costs, unless they see a provider who is out of network.
Uninsured or underinsured Americans will have access to free shots as part of the Biden administration’s “Bridge to Access” program, which will keep a limited supply of vaccines and therapeutics on hand to distribute free through state and local health departments, as well as pharmacies. But, they may not be available at pharmacies until mid-October at the earliest.
Some experts said they are worried a lot of people may fall through the cracks in the system. Just because the vaccine may be available doesn’t mean getting it to people will be easy. The uninsured may not know how to get the vaccine, or even that it’s available.
“I think that there’s going to be vaccine available, but it’s not going to be what people saw before because there’s going to be more and more hoops to jump through,” said Bruce Gellin, chief of global public health strategy at the Rockefeller Foundation.
“And that’s going to make it more complex, which then gets back to how clear the messaging is for people [about] what they’re supposed to do and what they’re supposed to expect when they go to the same place they went before, but it’s not the same drill,” Gellin said.
A Moderna spokesman said the company is working with the government on the “Bridge” program, but did not provide more details.
Some people without insurance may be able to get boosters free from safety net providers, but others may have to pay the full cost.
Updated at 4:05 p.m.